Vik: Thank you so much for attending this course. I hope we can make this a very collaborative and educational type of session.
Severe Multiple Sclerosis (MS)
Severe multiple sclerosis is a progressive form of MS with no periods of remission. MS can affect all areas of daily living including activity demands and occupational challenges in work, leisure, and quality of life. The videos and images depicted within this presentation are of actual individuals who have MS, particularly the primary progressive type, and they require total assistance throughout all areas of ADLs and IADLs. They may be non-verbal, which most of them are, have dysarthritic speech, or require a motorized platform for functional mobility. I am extremely excited to present actual case studies of actual individuals, particularly within the VA system of New York, who are enduring the symptoms of MS and who have agreed to share their experiences. I have gained consent from every single individual for educational purposes, while still adhering to HIPAA mandates.
Disease Progression
MS still has an unknown etiology according to research (www.nationalmssociety.org). It affects both men and women, and there is no true single diagnostic tool or test for diagnosis. Diagonsis is based upon symptoms and after everything else is ruled out such as: Parkinson's, fibromyalgia, or other neurological insults. Symptoms are usually evident in young adulthood; however, research has shown that pediatric MS can emerge before age 18. There is a disruption of communication between the central nervous system (brain and the spinal cord) and the rest of the body (peripheral nervous system). It is not a fatal disease and it is manageable, but there is no cure. There is active and aggressive management of the disease. Someone suffering from MS can still live a normal life expectancy, but other comorbidities and complications may play a role. There are 4 major categories of MS.
Symptoms of MS
There are many symptoms of MS (www.msfocus.org).
- Fatigue
- Weakness
- Tone
- Visual deficits
- Cognitive deficits
- Bowel/Bladder capacities
- Emotional changes
- Communication
- Gait abnormalities
- Respiration
- Auditory deficits
- Sexual deficits
Fatigue is probably the most common and a very big deal. It affects every area of activity tolerance. Threapists commonly employ "energy conservation strategies", "activity modification", or "joint protection" strategies when treating fatigue. We do a vigorous activity analysis to see what steps can we remove from an activity to make it easier for the client. Weakness is another area that goes along with fatigue.
We often see a fluctuation of tone between low and high. There is no clear abnormality in tone for an individual with MS as every individual is different. I usually see high tone, especially with the presence of tremors, both resting and intentional, but I typically work with individuals that have a very aggressive form of MS and not the acute form.
There can be visual deficits as well. Within my practice, I often see a condition called optic neuritis, an inflammation of the optic nerve that causes impairment in visual acuity. It can cause blurry vision and an impaired visual field. Similiar to rheumatoid arthritis, there are going to be flare ups with optic neuritis, but there is management with medication. Individuals can also have nystagmus, or saccadic movements, and double vision.
There are also cognitive deficits, impaired bowel and bladder capacities, and emotional changes. Emotional changes can impact an individual's lifestyle. These emotional changes include anxiety, depression, frustration, lack of coping, and so forth. Remember to look at the clients holistically as they are going to have issues physically, neurologically, and psychosocially. Communication issues, gait abnormalities, respiration issues, auditory deficits, and sexual deficits are other symptoms seen.
The symptoms can change as the disorder progresses.
- Fatigue-Poor activity tolerance
- Weakness-Generalized weakness
- Tone-Tone fluctuations
- Visual deficits-Optic neuritis
- Cognitive deficits-Depression, paranoia, poor recall
- Bowel/Bladder capacities- incontinence
- Emotional changes-mood disorders
- Communication-non verbal
- Gait abnormalities-wheelchair dependent
- Skin breakdown-pressure development
Over time, the symptoms begin to take over a person's lifestyle, especially the major symptoms of fatigue and weakness. Poor activity tolerance and general weakness are chief complaints. Every joint does not feel 100%. Bowel and bladder capacities change, and incontinence can become a problem. Prolonged incontinence can then cause skin issues and pressure sore development. Communication also becomes very difficult. They can have dysarthritic speech, and it takes increased effort for them to speak. Emotional and cognitive changes can continue to progress and transition into depression, paranoia, and poor recall, especially during the late stages of MS. All of this can affect their self-image.
Assistive Technology (AT) Considerations
There are many assistive technology considerations.
- No technology, low technology, high technology
- Longevity of the chosen form of technology
- Burden of care
- Context adaptability
- Model of practice (HAAT Model)
- Simplicity/complexity
- Safety
- Situation specific or diversified use
With my work within the veteran population, I have found that towards the end stage of MS or when symptoms really become dominant, it is no longer about simple access or ADLs and IADLs, but it is more about quality of life. With a push for client-centered care, you have to consider what they want to do. By developing good rapport therapeutically, it is going to make treatment a whole lot easier.
We need to look at whether the client needs technology. No technology might be more beneficial than considering low or high tech at all. Sometimes therapists push technology too much, too fast, or too aggressively. We also need to look at the longevity of the chosen form of technology. How can I make my recommended AT, whether it be something as simple as a sock aid or a reacher (low tech), or as complex as a communication device or head array controlled motorized wheelchair (high tech), last as long as possible? This is when your clinical reasoning comes in. You need to think about how the person will interact with this technology within their context.
There is a model of practice within AT called HAAT, Human Activity Assistive Technology model. It is similar to our other occupational therapy framework models, MOHO and PEO, but within this specific component, it looks specifically at AT and the human components of client factors, performance skills, and context.
We also need to look at the simplicity or complexity of a device. If it is too complex, they may abandon the equipment, or lose interest if it is too simple. Safety is also a huge concern. Finally, does the recommended AT have one specific use or could it be adapted and modified for an array of contexts? Use in a multitude of ways is always going to be a plus when it comes to reimbursement.
Low Versus High Tech
Low tech can include modified tools to assist in ADLs and IADLs, that can be easily manipulated and controlled by the individual with MS, without a huge array of knowledge or burden of use. High tech can include an interface which requires training and education, and a period of acclimation to execute the higher levels and demands of task performance.
Video 1
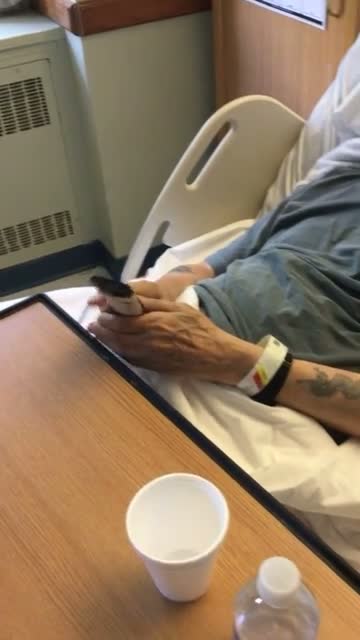
In this video, are we looking at some type of resting tremor or intentional tremor? This is an older individual with MS, and his symptoms are going to be a lot different than the other videos you are going to see. He has a lot of resting tremors. In this picture, there is a lap tray, a cup, and a bottle of water. Do you think he is going to be able to independently pour this bottle of water into the cup without a huge amount of spillage? There are several options that we can use to intervene in this situation. Dysem might help to stabilize the cup, or a weighted cup with two handles might help. Using both hands to grab that cup while also providing some proprioceptive input might make it a little bit easier for him. Other options are a sippy cup or a nosey cup to prevent spillage. He is right hand dominant so we definitely want him to use both hands to grab that cup. My point is that when it comes to low tech items, there are an array of strategies and devices that we can use in the presence of tremors.
Video 2
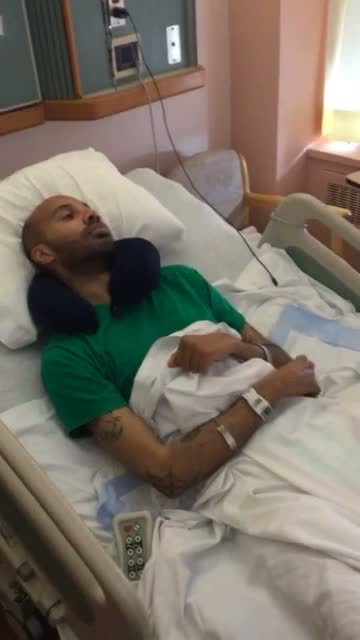
This is an individual with intentional tremors. This individual has MS, the primary progressive type. He is trying to grab his phone on his left side, and you can see that it is not an easy task. We see a lot of incoordination happening here. When it comes to high tech devices, there are any array of options. Right off the bat, we look at something as simple as a mounting device. We could use a simple mount for his phone on his dominant side. A mount could increase the predictability of where his phone is going to be. Is anyone concerned about safety? Do you think the force or the velocity of how fast his hands are moving might have an impact if he were to try to bring the phone to his ear? To compensate, we could use a simple goose neck mount with an extension onto one of the bed rails within his visual field. I think that would increase the predictability where his phone is going to be, while it will also increase his safety.
Resources for AT Acquisition: Low/High Tech AT
Here are some wonderful resources for AT when it comes to the acquisition of low and high tech items.
Switches/Mounts/ECU’s/Home Modification:
- EnableMart-Assistive Technology: https://www.enablemart.com/
- Assistive Switch Laboratories: http://www.asl-inc.com/products/new-products.php
- Adaptivation Incorporated: https://www.adaptivation.com/
- Ablenet: https://www.ablenetinc.com/
These are national resources. I have had great results with all of these. They also have online support and chat. You can speak with an assistive technology professional (ATP) if available, or they can come out and perform an assessment. As an ATP myself, I have a hard time keeping up with the endless amount of resources that are available, and I rely on the manufacturers and vendors to keep me up to date. You always want to give your client the newest AT version, with less bugs.
This is a list of resources for seating and mobility needs.
- Sunrise Medical: http://www.sunrisemedical.com/
- Ki Mobility: http://kimobility.com/
- PDG Mobility: http://www.pdgmobility.com/
- BRODA Seating: https://www.brodaseating.com/
- Quantum Rehab: http://www.quantumrehab.com/
My specialty is seating and mobility. I enjoy looking at a complex seating system and breaking it down to see if it matches my client's needs. I have found great success with these companies. Again, these are all national. I am not supporting one over the other as they all have their specialties. I have images to support what each company has to offer, and you as a clinician can make your choice.
Seating and Mobility Considerations
Here are some considerations with seating and mobility.
- Thermoregulation
- Pressure relief
- COMFORT!
- Static or dynamic system?
- Motorized, non-motorized?
- Independent, attendant mobilization
- Durability
When they are dependent in their seating system, thermoregulation can become an issue. When they are sitting for a long period of time in a seating system, they can overheat in the regions of their ITs and mid to lower back areas. This is a huge risk factor for pressure ulcers. Often clinicians overlook this factor. We also have to have a means for pressure relief through either a static or dynamic system, or a motorized or non-motorized system. Another huge issue in this population is comfort. We need to gauge the comfort of a person using a subjective response mechanism and not only through objective data. "I am not comfortable." "I have pain." What if they cannot verbalize to you? You can use facial expressions or some other type of non-verbal scale. I also use a pressure mapping system to make sure that I am objectively getting an even distribution of pressure. Comfort is a huge factor that I consider when assessing someone's seating and mobility needs. I want to make sure that they are comfortable so that they can be functional in my recommended system.
Dependent Seating Systems
Here are some dependent seating systems shown in Figure 1.

Figure 1. Examples of dependent seating systems.
The first system is a BRODA seating system in the top left. This has both a tilt and recline system for comfort. The wheels are located very far back to increase stabilization, especially if there is an active tremor involved. This is not self-propelling. Looking at the front casters, this is also not going to be ideal for outdoor use as it will not roll smoothly. This is more of an institutional setup. There are side bolsters, side lateral supports, and a head support.
The picture in the middle is of a tilt/reclining wheelchair. Looking at the rear wheels and how small they are, you can determine that this is also not for self-propelling, thus it is a dependent system. We could always change out the rear wheel and get a larger wheel if appropriate. With the smaller wheel, it is easier to maneuver this wheelchair within an institutional setting. There is also an aggressive four-inch cushion, deep laterals, and a head support for increased comfort and posture.
The far right picture on top is the same type of chair, but it is from a different company. As you can see, it has much larger rear wheels and can be tilted.
On the bottom left is a similar wheelchair as the one in the middle except that it can tilt the person with a switch. You can mount a switch anywhere it is accessible, and then the client can alleviate pressure themselves. There is also an attendant-operated tilt as shown on the right.
Independent Seating Systems
Independent seating systems are shown in Figure 2.

Figure 2. Independent seating systems.
This first chair (on the far left) is an E-Motion chair which is a semi-motorized platform. The wheel has a built-in motor, and it creates an equivalent or less-than-equivalent amount of torque. This helps address fatigue and discomfort. The next wheelchair to the right is an ultra-light manual wheelchair. This is a very light model, usually less than 37-38 pounds with all the accessories. This is meant for pure mobility. The next chair to the right is called an E-Motion wheel. These are extender wheels from Sunrise Medical, an amazing option for someone who wants to go long distance without the fatigue. This is the same concept as the E-Motion chair, but the battery is located towards the back on this model, whereas in the far left picture, the battery is located towards the center hubcap. In order to charge the battery, you need remove it and charge it on a docking station. In the E-motion wheel, you charge directly into the wheel. Some clients and their caregivers are not able to remove the battery so charging within the wheel is a better option. Lastly, on the right, we have a tilting/reclining wheelchair with a moveable axle. This wheel can go forward and back to allow better hand-rim control.
Motorized Mobility
Let's take a look at motorized mobility.
Video 3

This is the same individual that was attempting to grab his phone. He is being trialed on a mid-wheel drive motorized wheelchair with a right-hand joystick control. In this video, you can see that he needs his head positioned better for visual access of the environment.
