What We Are Covering
- Mobility Series
- Augmented Mobility
- Dependent Mobility
- Manual Mobility
- Power Mobility
This is part of a series on mobility. Mobility devices are on a spectrum. We start with augmented mobility devices like canes, crutches, walkers, and gait trainers. From there, we move into dependent mobility devices such as adaptive strollers, transport chairs, and tilt-in-space manual wheelchairs. Manual mobility and power mobility devices round out the series. We have courses on each of these topics. If you are interested, I encourage you to check out each of these.
Augmented mobility uses devices that augment or assist ambulation. These are used with someone who has some ability to ambulate. A device augments mobility to either improve efficiency, safety, or both. This includes walking aids such as canes and crutches, walkers, and gait trainers. These are each used for different reasons with different ages, populations, and diagnoses. We will touch on this as we move through this information.
Why Does Someone Need These Devices?
- Decreased strength
- Decreased balance
- Decreased stability
Why does someone need these devices? It could be for a host of reasons. Many of us have used a pair of crutches or maybe even a cane. You may have sprained your ankle or broken your leg. These are fairly familiar pieces of equipment to us and are often used temporarily. People who may need to use these on a longer-term basis may have decreased strength, decreased balance, or decreased stability.
Goals of Augmented Mobility
- Fall prevention
- Increased mobility
- Strengthening
- Dynamic weight-bearing
One big goal with using augmented devices is to prevent falls by compensating for lack of strength or balance. We also want to increase their mobility, so this person can go a little further or ambulate in other environments than their home. Many people "furniture walk" in their home, which we know is not very safe and certainly limits where they can move. Sometimes, this equipment is used for strengthening to improve functional abilities. Again, it depends on the item and the person using it. Some of this equipment, particularly gait trainers, provides dynamic weight-bearing, rather than static weight-bearing, like in a stationary stander. The person moves while bearing weight through their legs.
Who Uses This Technology?
- Varies with device
Who uses these devices varies by device. We will talk about people who use these in each of these categories of augmented mobility as we go.
Canes
- Definition
- Types
- Clinical indicators
- Contra-indicators
- Population
- Clinician role
We are going to start with canes. You may be thinking, "I know what a cane is. How hard can this be?" There are times when it is appropriate for a client to use a cane and times where we should be recommending something else. And, there is a surprising amount of variety of features on canes that can make a significant functional difference to the client.
Definition
- A cane is generally a vertical pole with a handle grasped by one hand to assist in ambulation.
Types
- Standard canes
- Typically, height adjustable
- Quad canes
- Seat canes
- Walking sticks (1-2)
We have all seen those standard canes. These are typically height-adjustable, designed to be rather generic, and are typically accessible at local drugstores. They are designed to meet many people's needs. These are height-adjustable to find the correct height for an individual. This is based not just on their own height but also on whether there is some fixed kyphosis happening or other factors to best support the individual. There are quad canes like the one pictured in Figure 1.

Figure 1. Quad cane from ProBasics.
The idea is to provide more stability under the cane than one single point of standard cane. There are seat canes. These are a little clunky to use as a cane, but the idea is that if someone gets tired, they can stop and sit down.
Some people benefit from using walking sticks. I use a walking stick when I am hiking. These are also height-adjustable, and a person might have better control with a walking stick, particularly if they need that height to be much higher than a standard cane.
- Accessories
- Flex tip
- Self-standing tip
- Ice cane attachment
There are also a variety of accessories for canes. In Figure 2, there is a flexible tip that is available from many manufacturers. This means that when I put my cane down, even if the cane is not absolutely perpendicular to the ground, the tip of that cane will be firmly in contact with the ground because it flexes. This can really help someone be safer as it improves stability. Figure 2 shows a self-standing tip.

Figure 2. Flexible cane tip by FlexSTICK company.
It depends on the cane's surface, but this helps someone be less likely to drop their cane. For example, a person can put their cane down to unlock their front door. They do not have to worry about leaning it up against something and it slipping. This can be a common concern. There is even an ice cane attachment that you see pictured in Figure 3.

Figure 3. Ice cane tip by Vive Health.
I would be a little leery of recommending that my clients go out with their cane in an ice storm. However, if the conditions are such that this type of tip is required to improve safety, it is available.
- Features
- Folding
- Various style handles
There are folding style canes. If someone does not need their cane all the time and wants to fold it up to stash it in their purse or bag, it gives them that option. This is also a convenient option when traveling, especially on airplanes. There are different handles too. Some of these handles are designed to look a little more interesting, while others are designed for specific ergonomic purposes. Depending on your client's grip or range limitations, different styles can be used to best match the person's abilities.
Clinical Indicators
- To provide walking assistance
- To assist sit to stand
- Temporary use: post-injury or surgery
- Long term use: decreased mobility
Canes provide walking assistance as someone is moving along. They can also assist in sit to stand if done safely. It depends on the individual client. It might be that the cane is used only temporarily after an injury or surgery. For long-term use, it is appropriate for someone who has some decreased mobility.
Contra-indicators
- If a client requires more support
- Putting too much weight on the cane
- If a client requires more stability
- Risk of falling, even with the cane
When do we not want to use a cane? If the client requires more support and is putting a tremendous amount of weight on the cane, it will be difficult for them to use the cane functionally, and they are more likely to fall. It could be the client is stabilizing too much against this cane. We may need to distribute that pressure out a little more. If the person requires more support or stability, there is a risk of falling even with a cane. Now, it becomes something they can trip over. In these cases, we may want to look at a different mobility category.
Population
- Stroke
- Diabetes
- Multiple Sclerosis
- Obesity
- Others
Who uses canes? People who have had a stroke, where one side of the body is more involved than another, may use a cane on their non-involved side to compensate for the involved side. People with diabetes may benefit from the use of a cane. People with multiple sclerosis may also use one, depending on their level of involvement. Additionally, people who are obese may benefit from the use of a cane. It also does depends on whether this is a permanent or temporary situation for the individual.
Clinician Role
- Determining if a cane is appropriate
- If so, determining the style of cane, including handle and base
- Determining the best height for the client
- Training
What is our role as a clinician? We need to determine if a cane is appropriate versus another category of augmented mobility, such as crutches, walkers, or gait trainers. If we determine that a cane is appropriate for a client, we need to determine cane style. Do they need a standard cane, a quad cane for more support, or even a walking stick or a pair of walking sticks? Once we have determined the cane style, we also have to determine the best handle and base or tip. The majority of clients are going to use a standard cane. Often, clients like these better due to aesthetics. However, for some clients, the aforementioned options/accessories can improve their safety and efficiency.
We also have to determine the best height for the client. Again, this is not simply a formula of how tall the client is. We might have to try several heights to determine how the height affects someone's posture. We do not want someone to end up bent over further than they need to be. Conversely, if the cane is too high, it may be difficult for someone to stabilize against. We may have to try several heights and observe how that person walks with that particular height configuration. We want to observe their posture, the efficiency of their gait, and how much they stabilize against the cane.
Even though a cane may seem like a simple thing, training is important. We have to determine if the cane is used to mimic the leg's stride closest to the cane or of the opposing leg? This is going to depend on the individual's needs, and that is something that requires some further assessment as well as training on our part. Training should include getting up and down from surfaces and up and down stairs. These are all things to keep in mind.
Crutches
- Definition
- Types
- Clinical indicators
- Contra-indicators
- Population
- Clinician role
Many of us have used crutches. Perhaps, you had to use crutches (one or two of them) for a short period of time after you sprained your ankle or broke a leg. Some of our clients need crutches for a longer period of time.
Definition
- Crutches are often used in pairs to transfer weight from the legs to the upper body
Crutches are often used in pairs. It can be challenging to transfer weight off of the legs. There are many different styles. It is exciting to see some product innovation on standard crutches as they have not changed in a really long time. Standard crutches are difficult to use because they tend to create a lot of weight in the axilla depending on the height and how they are adjusted. There is also a tremendous amount of force that goes through the wrists and shoulders during the management of these.
Types
- Types
- Standard
- Lightweight
- Ergonomic
- Forearm
- Specialty
There are have standard crutches. There are lighter-weight crutches, even though standard crutches are fairly lightweight if they are aluminum versus wood. There are also ergonomic options like the one pictured in Figure 4. This uses a different type of design to make use of the crutch less detrimental to the shoulders and the upper extremities as a whole.
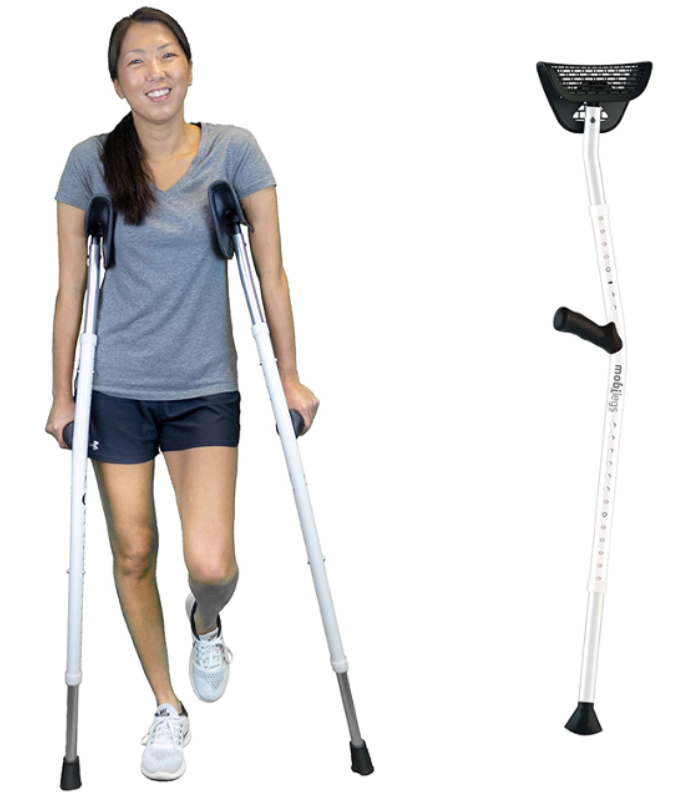
Figure 4. Ergonomic style crutches by Mobilegs.
There are also forearm crutches like the ones in Figure 5. The design of forearm crutches has not changed a lot over the years, but there has been little improvement.

Figure 5. Forearm crutches by Medline.
These are typically used by people who need a crutch for a longer period of time.
There are also a variety of specialty crutches. Figure 6 is designed for someone who cannot put weight on one foot but can bear weight through the upper leg, knee, and foot. They can use this scooter-type crutch to support their affected leg and move the device with the other leg.

Figure 6. Specialty "crutch" by Drive Medical.
Figure 7 shows a similar option for people who can bear weight through the hip and knee but not the ankle and foot. This is called an iWalk.

Figure 7. Hands-free crutch by iWalk.
It is attached to the client's bent knee, and the person can use it to walk hands-free. I personally do not think I would do well with that style.
Clinical Indicators
- Short term injuries, post-surgery
- Long term mobility limitations
Crutches are typically indicated for short-term injuries and post-surgery, especially for those standard crutches. Long-term mobility limitations may indicate the use of crutches as well.
Contra-indicators
- If the client requires more support
- Inadequate upper body strength
- If the client requires more stability
- Fall risk
- Long term use can lead to excessive stress at the axilla, shoulder, elbow, and wrist
When would we not use a crutch? Here is another more ergonomically designed crutch in Figure 8.

Figure 8. Ergonomically designed crutches by LifeCrutch.
The client may require more support than the crutch provides. This could be the case for clients who do not have much upper extremity strength, like the geriatric population. It is tough to support a large percentage of your body weight using your arms. They may also require more stability than crutches can provide. Long-term use of crutches, depending on the style of crutches, can also lead to excessive stress at the axilla, the shoulder girdle, the elbow, and the wrist.
Population
- Short term use
- Post-injury
- Post-surgery
- Long Term
- Cerebral palsy
- Spina Bifida
Who uses these? For short-term use, it could be any of us for post-injury, post-surgery, et cetera. People with cerebral palsy or spina bifida may use these if they have some ability to ambulate. Typically, clients with these conditions would use forearm crutches.
Clinician Role
- Determining if a crutch is appropriate
- If so, determining the style of crutch
- Determining the best height for the client
- Training
We need to determine if a crutch is appropriate for someone in the context of other augmented mobility device categories. I hope you can see that this can be a little more complicated than obtaining crutches at the local drugstore. If we do determine that crutches are appropriate, we need to decide on the style. A standard crutch would not be appropriate for long-term use. What type of crutch is going to meet this client's needs best.
We also have to determine the best height for the client. Again, this is not simply a measurement. For a sprained ankle, the height might be a simple measurement. However, there may be other considerations for clients who have motor impairments in determining the best height. There is also some training involved. We want to minimize the risk of injury to the client during crutch use.
Falling is when using crutches is really dangerous. We do not want our clients falling as it is, but if they fall while using crutches, they are at an even greater risk as they will have less ability to protect themselves with their arms.
Walkers
- Definition
- Types
- Clinical indicators
- Contra-indicators
- Population
- Clinician role
By the time we get to the walker category, clients may also be using other mobility devices. For example, an individual may use a manual chair for longer distances, but they may use a walker inside their home. It is important to keep in mind that context.
Definition
- Walkers provide support and stability during walking by transferring weight-bearing to the upper body and providing a wide and stable base.
Walkers provide support and stability during ambulation, similar to a crutch. Depending on the type of crutch, sometimes we are unloading one side or one leg. We want no weight bearing on one leg, as an example. Both legs are being used with a walker, but some of that weight is being transferred to the upper body. The walker also provides a wide and stable base to prevent this person from falling.
Types
- Standard
- folding
- Rolling
- 2, 3, or 4 wheel
- Heavy duty
- Reverse
There are different types of walkers. There is a standard walker. These generally fold, making it really easy to throw them into the car. When the person is very active moving from location to location, there are rolling walkers. These come in two, three, or four-wheel configurations. For example, the walker could have two wheels on the front, like the one shown in Figure 9.

Figure 9. Walker with two wheels in the front from Drive Medical.
Figure 10 shows a three-wheel walker, and Figure 11 shows one with 4 wheels. These are all options from Drive Medical.

Figure 10. Three-wheel walker.

Figure 11. Four-wheel walker.
Three-wheel walkers have been top-rated lately. Some of these are heavy-duty for a bariatric client or are just hard on their equipment and need more stability. There are also reverse walkers where the walker is actually placed behind the client, and the client pulls the walker forward rather than pushes it in front of them.
Type: Standard.
- These require the client to lift the walker with each step
- This keeps the walker from rolling forward without control
- Lifting can lead to loss of balance and requires strength
- Standard tips can be replaced with skids or even tennis balls to allow the walker to be moved without lifting but without rolling
- These usually do not include a seat
- Folding
Again, standard walkers do not have any wheels on them, as in Figure 12.

Figure 12. Standard walker with no wheels from Drive Medical.
They require the client to lift the walker with each step. Whenever the walker is not in contact with the ground, not only is the client supporting the weight of the walker, but now they have lost their stability until the walker comes down and contacts the ground again. There are definitely some drawbacks to this, depending on the client. This is similar to the task of walking. I remember hearing from someone a long time ago is really controlled falling. We lift our foot, move it forward, and then land on it to prevent us from crashing to the ground. Moving a standard walker is similar.
An advantage of a standard walker is that there is the resistance of the walker against the ground. It keeps the walker from rolling forward. Some will attempt to push it forward against the ground and use that resistance. This sometimes works, and sometimes it does not. It really depends on how much weight the person is putting on the walker and what surface they are walking on. It also does not work too well on the carpet. Lifting can lead to a loss of balance and requires a certain degree of strength.
The standard tips can be replaced and often are. We can replace them with a skid, like the one shown in Figure 13.

Figure 13. Walker glides.
This allows someone to slide over a surface, even carpet more readily. Many people will also cut a notch in a tennis ball and put these on the tips. It provides some resistance so that hopefully, the walker will not get out of control as someone is moving along. It allows the walker to keep moving without being lifted. These standard walkers do not usually include a seat. However, they do typically fold and are height-adjustable to meet someone's needs best.
Type: Rolling.
- Sometimes called Rollators
- 2 or 4 wheels
- Many fold for transportation
- Rolls to avoid lifting
- Brakes allow the client to control resistance
- Seat usually included if the client needs to rest
Rolling walkers are sometimes called rollators. These include two or four wheels. The one shown in Figure 14 has four wheels.

Figure 14. Rolling 4-wheel walker with a seat.
The two-wheeled option provides a little more resistance so that the walker does not get away from someone, particularly on smooth surfaces where the client could be at risk of falling. Many of these also fold for transportation. The ones with a seat allow the client to turn around, sit down, and rest. The one in Figure 14 has a seat that lifts with a convenient storage area underneath. For folding, the seat generally has to be lifted to allow this to fold side to side.
By rolling, we avoid the lifting that occurs with a standard walker. Often, there are brakes on these wheeled walkers due to the four wheels, as it is very easy for this walker to roll away from someone on a smooth level linoleum surface. The client can hang onto those breaks to provide a little bit of resistance while walking or stopping. The client has to have an adequate grip to hold on to the brakes. As you can see in Figure 14, there is quite a spread between the grip and the brake so that the client may have difficulty with this.
Type: Reverse.
- Often used in pediatrics
- This configuration may encourage ambulation for certain clients
- Promotes extension and stability
There are also reverse walkers like this one shown here from Kaye Products.

Figure 15. Reverse walker configuration.
This is often used in the pediatric population. It can support and encourage ambulation in certain clients. Part of the reason is that it promotes extension because of the placement of the walker. Whereas, when we have a walker in front of us, even though our hands seem to be in the same position, oftentimes, this causes more flexion of the trunk. We can address some of that with the height of the walker. It is important again to determine the best height for an individual. This might mean we need to change the height either higher or lower to promote an upright posture and optimal stability. We also need to ask the client what height they prefer. The client might have a "sweet spot" where they feel most comfortable.
Accessories
- Forearm supports and hand grips
- Wheels
- Size
- Locking or swivel
- One-way wheels
There are a lot of accessories that are available on walkers. The vast majority of people who use a walker can use a standard or rolling walker. However, some clients need more accessories to help with their unique issues.
First, there are forearm supports and hand grips. An option is in Figure 16.

Figure 16. Forearm supports and hand grips on a walker by Costway.
This gentleman is resting his hands in a forearm trough that provides stability. He may need these because he does not have much control of his hands or good hand strength. The grips can also provide stability or provide a different orientation for a better grip. Instead of holding that grip parallel to the floor, now they can hold the walker perpendicular. These are often angle adjustable as well. Thus, we can place that grip where someone has the best control, and they do not need to be the same on each side. It might be that someone needs a different angle grip on one side of their body than the other. You can see this still allows us to use it on a height-adjustable walker. Some walkers will include this as an option, and some do not. We can choose different sizes of wheels, as the example in Figure 17.

Figure 17. Adjustable wheels by Drive Medical.
We can choose different sizes of wheels. The smaller the wheel is, the more maneuverable the walker may be in terms of turns. However, it might get hung up on little things much easier. If the wheels are larger, it might turn in a little bigger radius, but generally, it will be easier to overcome carpet or thresholds. Wheels can also swivel or lock. If they lock, the wheels will only roll straight ahead. This might be optimal if someone is having difficulty maintaining a straight-ahead orientation. For example, someone who has had a CVA may tend to push more on one side than the other. We can lock the casters to try to help them stay on a straight course. Of course, that makes turns more difficult. The client may have to lift the walker to turn. It could be that you use the locking wheels initially with a client, and as they progress in strength and stability, you can revert to a swivel orientation. There are also one-way wheels that keep the person going forward but do not allow them to back up. This can be helpful for clients who have that particular challenge when using a walker.
- Seat
- Light
- Parkinson’s
- Trays, baskets, cup holders, etc.
- tipping
There are some other interesting accessories. This one always intrigued me in Figure 18. You can see it has a laser beam.
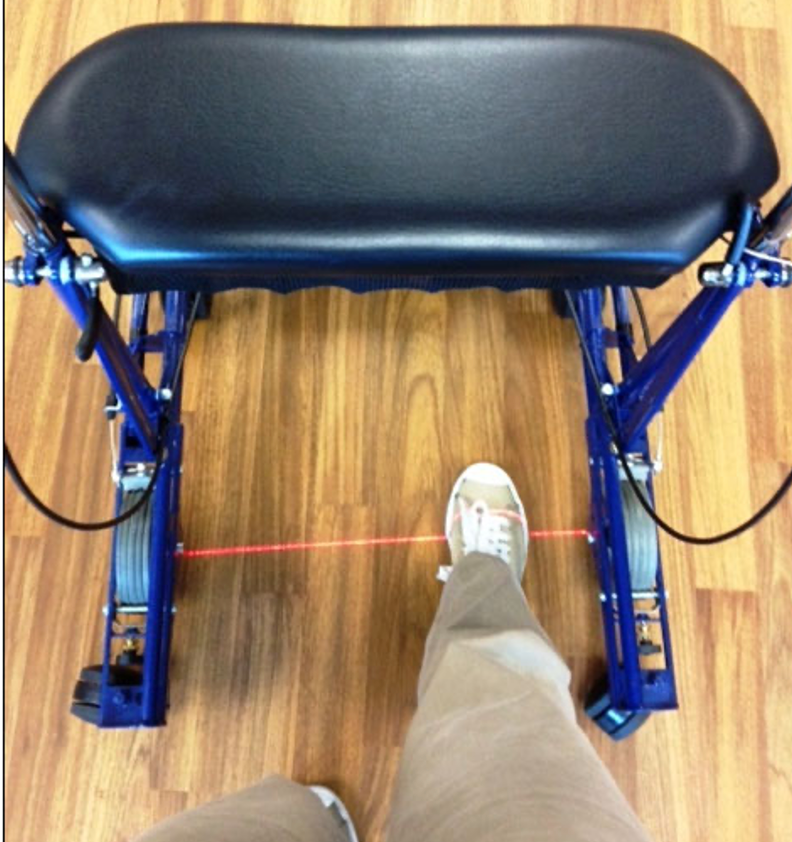
Figure 18. Walker with a laser beam light.
People with Parkinson's often have a terrible time initiating movement. You may have someone with Parkinson's who can stand in front of the walker but just cannot get it going. They need a lot of cueing to start that movement. With this type of walker, the person sees that light and moves their foot towards it. This can be really helpful to help those clients initiate movement. It gives them a target to go towards and can be very effective.
Many walkers have a seat as well. If the client is walking and becomes fatigued, they can sit down. Usually, the client does have to turn within the walker to find that seat which can be challenging. They have to let go of one hand and turn, and there is a risk of falling during that maneuver. That may require some specific training.
And then there are all sorts of trays, baskets, and cup holders. People who use walkers often are moving something with them from place to place in their home. As such, they may want to take a cordless or cell phone, a remote control, or a glass of water. The aforementioned accessories can be beneficial with these tasks. However, it is important to look at what is attached to the walker because sometimes it can make the walker tippy due to the added weight. I have seen some people really load down their walkers.
Clinical Indicators
- For clients who need more support and/or stability than provided by canes or crutches
- Short term or long term use
These are for clients who need more support and stability than is provided by any of the canes and crutches that are available. This might be used only short-term for someone who needs it as in a post-surgery or for a medical condition where the person recovers beyond the need to use this device. It might be that the person requires the device long-term. It is important to keep in mind these clinical indicators because if this is for longer-term use, we may have to consider other features than if only for the short term.
Contra-indicators
- When this level of support and stability is inadequate for a specific client
- Fall risk
- Typically, if this is inadequate, the client will require a wheelchair.
Walkers are not indicated when there is a high level of support and stability needed. If a client is still at risk of a fall, we need to look at something else. Typically, that is going to be a wheelchair. If someone falls and they have a walker in front of them, they will fall on the walker most likely, unless they fall rearward, which can lead to even more injury.
Population
- Geriatric
- Multiple Sclerosis
- Cerebral Palsy
- Others
Who uses walkers? Walkers are very common in the geriatric population. As people lose some muscle strength and need a little extra help, walkers can help them to stay mobile and as independent as possible. Also, walkers may be used by people with multiple sclerosis, cerebral palsy, and many others.
Clinician Role
- Determining if a walker is appropriate
- If so, determining the style of walker and needed features, accessories
- Determining the best height for the client
- Training
We need to determine if a walker is appropriate. If we do determine one is necessary, we need to determine the style of the walker, needed features, and accessories. We need to determine the best height for the client and then train the client in the use of the walker in all the environments that they need it in, including transferring to and from various surfaces like in and out of bed or in and out of a chair. At this level of intervention, oftentimes, an equipment supplier becomes involved, especially if we are using a walker with someone who has more long-term disabilities and needs more features.
For more complex equipment, it is important to work with a supplier as they are very familiar with all the equipment options. They may have the ability to get you the equipment to trial with an individual to ensure that it meets their needs. The supplier can then submit their order form and your letter of medical necessity to a funding source to get reimbursement for these various walkers. If there is a problem with the walker, they can provide adjustment and repair as well.
Gait Trainers
- Definition
- Types
- Clinical indicators
- Contra-indicators
- Population
- Clinician role
Definition
- Gait trainers support the client in a standing position to augment mobility and to provide dynamic weight-bearing
Gait trainers support the client in a standing position and augment mobility. They help the person with ambulation and provide dynamic weight-bearing. Instead of a client who is simply standing in a stationary stander, they can move their legs. This has tremendous physiological benefits for many of our clients and provides much more postural support.
Types/Features
- Rather than various types, gait trainers offer different features, specifically different postural supports.
Gait trainers offer different features and different levels of postural support to meet an individual's needs. There are other unique features as well. For example, this Kid Walk gait trainer is a mid-wheel drive (Figure 19).
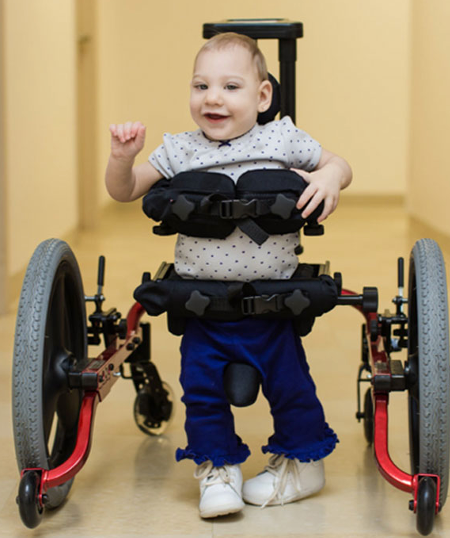
Figure 19. Prime Engineering Kid Walk gait trainer.
It turns right on the client's center. This can be helpful for some people who use gait trainers.
- Forearm supports, hand grips
- Provides upper weight-bearing and stability
As with walkers, we can add on forearm supports and hand grips. This provides that weight-bearing of the upper extremities to help compensate for less weight bearing through the legs. By bearing weight along the forearm, the client also gets a lot of stability through that area. We can also change the angle of the grip so that it best matches the client's ability. If the client does not have the ability to grip, they might still benefit from forearm support.
- Pelvic support
- Provides proximal support
We can also provide support at the pelvis. With a walker, the individual's weight is solely through their hands and maybe their forearms. With a gait trainer, we can provide more support for someone who cannot stand independently. We can provide different degrees of pelvic support to help someone assist with their ambulation. Figure 20 shows pelvic and trunk supports on the Grillo gait trainer. This can compensate for this person's lack of proximal stability.

Figure 20. Pelvic and trunk support from Ormesa Grillo.
- Seats
- For clients who cannot bear their full weight
They also have seats. This works well for a client who cannot bear their full weight. It compensates for someone's inability to put all their weight through their legs. There are all different types of seats out there. Some are rigid seats or even padded bars. This is more of a sling-style seat on the Ormesa Grillo in Figure 21.

Figure 21. Sling-style seating.
Often, they will not contact the seat. However, if their legs collapse or start flexing as they fatigue, then the client can bear some weight on the seated surface.
- Ankle Prompts
- Prevents scissoring, encourages alignment for ambulation
There are also what are called ankle prompts. You can see in Figure 22 that they are attached to the lower portion of the gait trainer and are straps that go around the ankles of the client.

Figure 22. Rifton ankle prompts.
These help to prevent scissoring. For example, a client with cerebral palsy may experience scissoring as they are walking. Their legs crossover each other due to excessive adduction and internal rotation. This prevents the client from moving too far and allowing them to move their foot forward instead of across. It encourages the alignment required for ambulation. While it might look like we have tied someone to their gait trainer, we are really attempting to prevent that excessive hip adduction.
- Trunk support
- Proximal support
In addition to pelvic support, we can also add trunk support, as in Figure 20. These are usually height-adjustable. We can choose how much support is required for an individual. This also allows for growth. Many children use gait trainers, and it is important to have built-in growth, adjustment, and flexibility as the individual grows and gains skills.
- Posterior Configuration
- Generally, less posterior support
There is a posterior configuration for many gait trainers, as seen in Figure 23.

Figure 23. Posterior configuration gait trainer by Drive Medical.
Generally, these provide less posterior support behind the client. Most of the support is in front of them for this young man. His support is primarily forearm supports and handgrips in this posterior configuration.
- Anterior Configuration
- More postural support options
In an anterior configuration, we can add more postural support options. You can see in Figure 24, the handgrips have been angled to meet this child's needs.

Figure 24. Anterior configuration gait trainer by Drive Medical.
We can also add on forearm supports and straps as needed. He has some trunk support here in front and behind him. In addition, he also has a seat to use when he is not bearing weight. He also has ankle props on here. This young man is demonstrating all the supports that you can add to this particular gait trainer.
- MidWheel Drive
- Allows for easier movement and turning
- More intuitive
- Suspension
I mentioned before that there is a mid-wheel drive option gait trainer. Figure 25 shows the Prime Engineering Kid Walk again.

Figure 25. Prime Engineering Kid Walk.
This allows for easier movement and turning of the base. It tends to be a little more intuitive because those wheels are really lined up with the client's center. It also has some suspension built into it. As the client takes a step, the gait trainer will move up and down slightly. This can be very helpful for some clients in assisting with the movement of ambulation. You can see that this has a tremendous amount of posterior and anterior supports available as the client needs it, including head support. Not all gait trainers provide supports that high up, but this particular one does.
Clinical Indicators
- To develop ambulation skills in young children
- To provide some augmented ambulation
- To provide dynamic weight-bearing
- Many advantages of weight-bearing
What are the clinical indicators of these gait trainers? We want to use these to develop ambulation skills in young children. This is often used for our pediatric population as a therapy tool. It provides some ambulation and dynamic weight-bearing. It helps with strengthening for bone density and improves digestion.
Contra-indicators
- If the client cannot bear weight due to limited strength or orthopedic limitations
- If the client has limited mobility in a gait trainer, they may also require other mobility options, such as a wheelchair.
We may not want to use the gait trainer if the client can not bear weight at all due to limited strength or orthopedic limitations. If the client has minimal mobility in the gait trainer, then they may also require other mobility options such as a wheelchair. Many people who can use a gait trainer use this really more for therapeutic benefits than true functional mobility. These do tend to be rather bulky, and if they are trying to move throughout their school or home, it might be a little cumbersome. Also, using this for long distances may simply not be practical for most people. Instead, it is typically used as a gait trainer during school or therapy or at home to strengthen and weight-bearing therapeutic goals. If the child is going to the zoo as an example, they would most likely use their wheelchair base.
Population
- All ages, but more so with children
- Cerebral palsy
- Developmental delays
- Other
Who uses gait trainers? All ages can use gait trainers, but we tend to see these used a lot in the pediatric population. This is commonly used in people with cerebral palsy and other developmental delays. There are a wide variety of options. We definitely want to work with the complex rehab equipment supplier to determine what options we have and what to include in the documentation to get funding. Gait trainers are getting a lot more expensive, and we want to make sure they will work for the client before we make a recommendation.
Clinician Role
- Determining if a gait trainer is appropriate
- If so, determining the style of gait trainer and postural supports
- Determining the best configuration for the client
- Training
- Ensure that mobility needs are met with other equipment in addition to the gait trainer, as needed
Our role is to determine if a gait trainer is an appropriate intervention for a client. We also need to determine the style of gait trainer and all those various accessories that are required. There are quite an array of postural supports to choose from. Depending on what accessory someone needs, like a head support, there are only a few gait trainers that offer that. We need first to determine all the features required to support this person for augmented mobility in a gait trainer and then which brand will offer all those. A supplier or manufacturer's representative can help with that particular recommendation. We then need to train this person to use it and train caregivers in how to place the person into the device accurately. We want to make sure that the mobility needs of the person are being met. Again, most people using a gait trainer are going to require another mobility device as well.
Resources
- For more information, check out:
- www.1800wheelchair.com/category/canes
- Canes, crutches, and walkers
- http://www.mayoclinic.org/healthy-living/healthy-aging/multimedia/canes/sls-20077060
- Tips for choosing and using canes
- http://www.emedicinehealth.com/crutches/article_em.htm
- http://www.mayoclinic.org/healthy-living/healthy-aging/multimedia/walker/sls-20076469
- Tips for choosing and using walkers
- http://www.especialneeds.com/adaptive-equipment-walkers-gait-trainers.html
- Paleg, Ginny. “Beyond Wheelchairs: Using Standers, Walkers, and Gait Trainers to Improve Mobility Problems.” Rehab Management. Nov. 2001: p.60+.
There are some resources that you might find helpful. If you look at 1800wheelchair.com (which is not where I suggest that we typically do our shopping), they list quite a bit of useful information about canes, crutches, and walkers. Remember that depending on the client, oftentimes, we can get funding assistance.
The Mayo Clinic has a beneficial article on the website listed here. This includes tips for choosing and using canes. This can be used as a helpful handout for a client. The emedicinehealth.com site has a digital article on crutches.
The Mayo Clinic also has a nice digital article on tips for choosing and using walkers and gait trainers. This tends to be a little more pediatric-focused.
One of my colleagues, Ginny Paleg, has a great article that came out in 2001. It is a very helpful article in Rehab Management. It is a little older but may have some useful information. She has some more focused articles that are more recent to that that you might want to refer to.
Hands-on Activity
- Borrow a cane, crutches, and a standard walker to try
- Use each device to move between rooms in your home
- List 3 motor skills required to use each augmented mobility device
And then I want to give you an idea of a hands-on activity. I suggest that you borrow a cane, crutches, and a standard walker and try them out. Use each device to move between the rooms in your home and analyze the activity with each device. List three motor skills required to use each of these augmented mobility devices as you move from location to location. How do they differ? What motor skills are required? What will help inform your practice as you specify a particular category of augmented mobility for your clients?
Summary
I want to thank you very much for attending this webinar. I also want to address a couple of common questions that people often have at this point. A very common question is around funding. Can I get this stuff funded, or do people simply go on Amazon.com and buy something? It is a little of both. If someone needs a cane or a walker temporarily, they may choose to simply rent one, borrow a friend's, or just purchase one on their own. Most funding sources will purchase this equipment for clients who need a piece of equipment for a longer period of time. Some of this equipment is considered to be more of a medical supply versus a complex rehab device. If it falls into a medical supply category, there may be a different supplier that the client needs to work through. It is important to make sure that we address the person's unique needs because many medical supply equipment options are extremely generic.
Once we get into more complex walkers and gait trainers, we must work with a complex rehab technology supplier. You can find suppliers in your area. Some of our main large suppliers in this country are New Motion and National Seating and Mobility. Contact them to let them know you need help evaluating a client or trialing some equipment. They will also help you to submit all the required paperwork so that funding can be secured.
If you have any more questions, feel free to reach out to me.
References
Available in the handout.
Citation
Lange, M. (2021). Augmented mobility intervention. OccupationalTherapy.com, Article 5415. Available at www.OccupationalTherapy.com
